Organ transplantation saves lives. According to the Organ Procurement and Transplantation Network, U.S Department of Health and Human Services, over 22,000 organs transplantation surgeries have been conducted between January and September 2016.
Ischemia Reperfusion Injury (IRI) is a well characterized cardiac transplantation-related complication wherein the host tissue (graft), deprived of blood supply for prolonged periods, undergoes damage when blood supply is restored post-implantation. Immune cells at the interface of the graft and recipient tissue mediate damage by releasing inflammation-promoting chemicals and free radicals.
In a study led by Nadig and colleagues at the Department of Surgery, Division of Transplant, Medical University of South Carolina, USA, researchers first acknowledge the central role played by endothelial cells (EC) in promoting IRI-associated tissue damage and subsequently developed a novel pH-sensitive, immunosuppressive drug-loaded, targeted micelle nanoparticle to curb the damaging effects of ECs. The team choose rapamycin as their immunosuppressive drug of choice given its dual roles in limiting cytotoxic immune cell functions and in protecting tissues that make up blood vessels.
While treating patients with immunosuppressive drugs prior to surgery is currently a standard practice, a major drawback of this approach is that these drugs prevent immune system activity throughout the body, placing patients at risk for diseases including diabetes and cancer. As an initial step in addressing this limitation, Nadig et al. coated the micelles with cyclic arginine-glycine-aspartate moieties, which specifically bind to and integrin protein (the alpha v beta 3 receptor protein) present almost exclusively on ECs. As a finishing touch, the team attached fluorescent chemical compounds to allow for tracking and visualization in their studies.
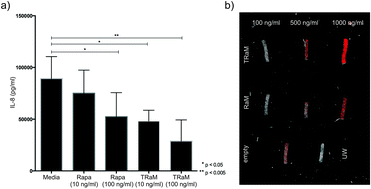
To demonstrate the clinical utility of their idea, the researchers exposed human endothelial cell cultures to hydrogen peroxide to mimic IRI-like conditions. The cells responded by increasing their production of inflammation-promoting chemicals. Importantly, the rapamycin-loaded nanoparticle micelles significantly curbed this response. Nadig et al. propose that the ultimate goal is to incorporate this technology into organ storage media to minimize the harmful effects of IRI.
Read the full article here:
RSC Adv., 2015, 5, 43552-43562
DOI: 10.1039/C5RA04057D